As a man ages, his prostate gradually grows larger. Although this enlargement is natural and generally harmless, sometimes it can indicate a serious problem. That’s why it is important for every man over 40 to learn about his prostate–what’s normal, what’s not, how to detect a problem and how to treat it. Here’s what you need to know now in order to head off trouble later.
Prostate problems are fairly common. Around the age of 50 about half of all men have difficulty because of the way the prostate grows with age. The prostate is a male gland, about the size of a walnut, which secretes a milky fluid needed for ejaculation. It lies at the base of the penis, just below the bladder and above the rectum, surrounding the first inch of the urethra (the tube that carries urine out of the bladder). Because of this location, growth of the prostate can cause the following common complaints:
- Weak or interrupted urine flow
- Difficulty in starting or stopping urination
- A need to urinate frequently, especially at night
- Pain or burning during urination or blood in the urine
- Inability to urinate
- Continuing pain in lower back, pelvis or upper thighs
If you have any of these symptoms, see your physician. Chances are you simply have an enlarged prostate, or benign prostatic hypertrophy (BPH). This condition affects 10 million American men. More than half of men between the ages of 60 and 70, and as many as 90 percent of men between the ages of 70 and 90, exhibit symptoms of BPH. The condition is not life threatening, but it can result in urinary tract infection and blood in the urine. Researchers are still trying to determine whether BPH increases the risk of prostate cancer, but so far there is no evidence that it does.
What Are the Treatment Options for BPH?
- Watchful Waiting. In most instances, symptoms resulting from prostate enlargement develop slowly, so living with the symptoms to see if they become less bothersome on their own is the first option. Men who have had bladder or kidney damage, repeated urinary tract infections or episodes of acute urinary retention may require surgery. But for the majority of men, the discomfort, risk and recovery period associated with surgery must be weighed against its probable benefits. Remember that the risks of surgery increase with age and the onset of other medical problems.
- Drug Therapy. Men with moderate symptoms may be given a drug that shrinks the prostate by blocking production of testosterone, the hormone that stimulates prostate growth. Researchers say about 70 percent of men who took the drug experienced relief. Some of its drawbacks: It takes four to six months before improvement occurs, it is expensive, symptoms generally recur once a man stops taking the drug, and it obscures prostate cancer test results. Other drugs which relax certain prostate muscles or reduce blood vessel wall expansion, can also be used to relieve pressure.
- Surgery. The most common surgical treatment for BPH is transurethral resection of the prostate (TURP), in which excess prostate tissue is removed using a tiny instrument inserted through the penis. A hospital stay of two to three days is usually required.
The success rate of TURP is high–about 85 percent–with only 15 percent of men needing a repeat TURP within 8 years. An estimated 400,000 TURPs are performed each year, making it the second most common procedure paid for by Medicare. But the surgery is not without side effects: Many men experience retrograde ejaculation, in which semen travels back into the bladder rather than out through the penis (though not medically harmful, it does render the man infertile). Also, about 4 to 8 percent of patients become permanently impotent.
Another form of surgery available is transurethal incision of the prostate (TUIP). In this procedure, the urologist passes a thin tube, or catheter, through the urethra into the center of the gland, then scrapes away prostate tissue with an instrument inserted through the tube. Rarely, this causes incontinence and impotence.
- Electrovaporization. This modification of TURP applies electronic waves through a device inserted into the urethra with a catheter. The waves vaporize prostate tissue.
- Needle Ablation. Transurethral needle ablation or TUNA was approved by the FDA in September of 1996 for the treatment of BPH. During TUNA, doctors heat and destroy enlarged prostate tissue by sending radio waves through needles positioned in the prostate gland. TUNA poses less of a risk of incontinence and sexual dysfunction than traditional surgery and can be perfomed as an outpatient procedure. However, it doesn’t reduce symptoms and increase urine flow as much as surgery does.
- Microwave Therapy. The Food and Drug Administration recently approved transurethral microwave thermotherapy or TUMT, a new technique that uses microwave energy to reduce the size and hardness of an enlarged prostate. Though TUMT does not cure BPH, clinical trial have shown it lessened the symptoms of 75 percent of patients treated with it. And so far the only notable side effect is that men are unable to urinate for several days immediately following treatment.
- Laser Therapy. A urologist inserts a laser into the urethra via a catheter. The laser heats and destroys prostate tissue, which the body eliminates over time. It may take several weeks to notice results.
- Balloon Dilation. This procedure is similar to the balloon angioplasty used to open up clogged arteries. Using a catheter, the doctor places a balloon in the part of the urethra that’s inside the prostate, then inflates the balloon to stretch the urethra. Improvement often lasts only one or two years, so balloon dilation use has declined.
- Stents. A tiny metal coil is inserted into the urethra to widen it and keep it open. Tissue grows over the stent to hold it in place. Stents may be recommended for patients who have a heart condition or other illness that prevents surgery.
- Experimental Treatment. The use of high-frequency, high-intensity ultrasound to destroy prostate tissue is being tested. The procedure is performed in much the same way as laser or microwave therapy.
Prostate cancer is the most common cancer in American men, second only to lung cancer as a cause of cancer deaths. In 1997, an estimated 334,500 men will be diagnosed with cancer of the prostate; 41,800 will die of it. Between 1980 and 1990 prostate cancer incidence rose 65 percent, largely due to improved detection.
However, a horde of uncertainties surround the diagnosis and treatment of the disease. Autopsy studies of men in their fifties who died of unrelated causes showed that one third had prostate cancer that was unrecognized during their lives. By the time men reach their eighties, it is believed 75 percent have some cancerous prostate cells. Still, nine out of ten cases of prostate cancer are “silent,” and grow very slowly. Consequently, it is said that more men die with prostate cancer than from it.
The challenge lies in identifying and aggressively treating the men at risk of dying of their cancer, while not treating those who may lead normal lives, unaffected by the disease.
The causes of prostate cancer are not known, but studies show it occurs mainly in men over 55–on average patients are diagnosed at 70. Having a family history of prostate cancer increases a man’s risk of getting it as well. The disease is also more common in black men. In fact, African-American men have the highest rate of prostate cancer in the world.
In addition, evidence suggests that a diet high in animal fat (including dairy products) increases the risk of death from prostate cancer. A recent Harvard study provides strong evidence that animal fats promote the development of prostate cancer and may be crucial in determining which cancers will change from a dormant condition to a lethal malignancy. Having had a vasectomy may also increase a man’s risk of prostate cancer. Two studies, largely financed by the National Cancer Institute, showed a slight statistical relationship between the two. But the data is far too preliminary to consider not having a vasectomy or vasectomy reversal.
Both the American Cancer Society (ACS) and the American Urological Association recommend yearly prostate cancer screening for men over the age of 50. A new study, however, challenges this advice. Canadian researchers warn that increased screening and treatment may lead to a poorer quality of life rather than a gain in life expectancy due to the possible side effects of surgery, including impotence and incontinence. Here, the screening methods that are currently used:
- Digital rectal examination. In this exam, the physician inserts a gloved, lubricated finger into the rectum and feels the prostate gland for hard lumpy areas. The problem with this method is that tumors may lurk in areas a doctor can’t reach. Also, many tumors are too small to be felt by hand. By the time a tumor can be felt, the cancer may already have spread to other parts of the body.
- PSA. This simple blood test measures levels of prostate-specific antigen (PSA) in the blood, high levels of which can indicate BPH or cancer of the prostate. Although studies have shown the PSA test to be the most accurate detection method, it misses up to 40 percent of prostate cancer cases and signals cancer in up to 30 percent of patients who are cancer free, leading to costly follow-up tests.
- Ultrasound rectal probe. This test uses sound waves sent out by a probe inserted into the rectum to form a picture of the prostate called a sonogram. Ultrasound can detect cancers that may have been missed in the above exams, but it is not regularly recommended for screening because of its expense and high rate of false positives.
How is Prostate Cancer Diagnosed?
If your doctor suspects cancer, he or she will probably refer you to an urologist, a doctor who specializes in diseases of the urinary tract and male reproductive system, for a biopsy. Performing a biopsy is the only way to make a definite diagnosis. How it works: the doctor removes a small amount of prostate tissue, usually with a needle, and sends it to a lab, where it is examined under a microscope to determine if the cells are cancerous. Often, a biopsy can be done in a urologist’s office, eliminating the need for a hospital visit. If prostate cancer is confirmed, the next step is to determine whether the cancer has spread beyond the prostate with more imaging tests. Doctors generally recommend therapy based on the stage of the disease, the patient’s age and medical history, the probable risks and benefits of treatment, the man’s ability to comply with treatment and his preferences.
How is Prostate Cancer Treated?
Deciding what is the best treatment choice depends to a great extent on the individual. It often comes down to trade-offs. Some believe the cure is worse than the disease, while others feel it is beneficial. After reviewing their options, many men with early prostate cancer decide to do nothing–the watchful waiting approach. A recent study by the Prostate Patient Outcomes Research Team of the Agency for Health Care Policy and Research found no clear benefit for aggressive therapy in many cases. The study found that prostate cancer may stay confined to the gland for years or even decades, making the severe side effects associated with treatment less worthwhile. See Guidelines for Watchful Waiting.
If your doctor and you decide intervention is necessary, radical prostatectomy, the surgical removal of the prostate, is one option. About 90 percent of these operations remove the cancer entirely. To determine if all of the cancer was removed, doctors monitor PSA levels after surgery. However, this surgery does have severe side effects: 40 percent of patients become impotent and significant incontinence occurs in 5 to 15 percent of cases. In addition, men who have this surgery no longer produce semen, so they have dry orgasms which, though upsetting to some, need not affect sexual pleasure.
Radiation therapy, the use of high-powered rays to damage cancer cells and stop them from growing, is another option. This is the best choice when the cancer has spread only to surrounding tissue and for older patients for whom surgery may be too dangerous. The side effects are: Impotence in 50 percent of men and incontinence in about 3 percent. Also, some cancer cells are left behind about 40 to 60 percent of the time.
What If The Cancer Has Spread Beyond The Prostate?
Neither surgery nor radiation is effective once the cancer has spread to the lymph nodes and/or bones. At this stage the main purpose of treatment is usually to curb the cancer’s growth and prolong life.
To accomplish this, doctors may recommend lowering testosterone, the male hormone that stimulate’s the cancer’s growth. One way to do this is through orchiectomy, the surgical removal of the testicles, which are the main source of testosterone. The side effects of this procedure include sterility and loss of sexual drive, usually accompanied by an inability to have an erection and hot flashes. An alternative to surgery is hormone therapy, which involves taking medication that counters the production of testosterone. Hormone therapy can cause loss of sex drive, erection problems, hot flashes, nausea or diarrhea.
In addition, chemotherapy, treatment with anticancer drugs, can reduce pain and other symptoms and slow down tumor growth.
Should I Get A Second Opinion?
Decisions about prostate cancer treatment are very complex and sometimes it’s helpful to have the advice of more than one doctor. In fact, many insurance companies require a second opinion before they will pay for the full costs incurred. If the second opinion contradicts the first, you may need a third opinion. A short delay in starting treatment will not reduce the chances of treatment success.
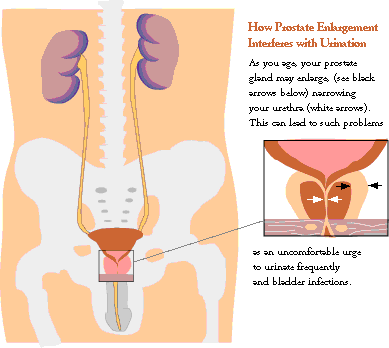
How Prostate Enlargement Interferes With Urination
As you age, your prostate gland may enlarge, (see black arrows below) narrowing your urethra (white arrows). This can lead to such problems as an uncomfortable urge to urinate frequently and bladder infections.
Patients generally want to learn all they can about their condition and treatment choices so they can take a more active part in decisions about their medical care. Since treatment for prostate cancer sometimes affects sexual activity and bodily functions, such as urination, it is especially important to weigh the risks and benefits of different treatments. Although written material is a good start, it cannot take the place of a discussion with your doctor. Your physician is best qualified to answer questions about the extent of the cancer, how it can be treated, how successful the treatment is expected to be and how much it is likely to cost. It is helpful to make a list of questions before you see your doctor.
Here are some issues you may want to discuss:
- What are my treatment choices?
- What are the benefits of each treatment?
- What are the risks and possible side effects of each treatment?
- How will the treatment affect my sex life?
- If I have pain, how will the treatment help me?
- Will I need to change my normal activities? For how long?
- How often will I need to have follow-up exams?
Taking notes can make it easier to remember what the doctor says. Some patients find it also helps to have a family member or friend along to take part in the discussion, to take notes or just to listen.
There’s a lot to learn about prostate cancer and its treatment. Don’t feel as if you need to understand everything the first time you hear it. You will have many opportunities to ask your doctor to explain things that are not clear. Use them.
Guidelines for Watchful Waiting
A recent Johns Hopkins study found that a combination of these two detection methods can reveal whether or not prostate surgery is necessary:
Calculation of PSA density. The amount of PSA in the bloodstream is divided by the size of the prostate (gauged by transrectal ultrasound) to determine how much PSA per gram of prostate tissue is produced. Based on this calculation, doctors can tell if high PSA levels result from a large prostate or a tumor that needs to be removed.
Evaluation of prostate tissue. In an outpatient procedure (sextant biopsy), six tissue samples from various sections of the prostate are analyzed. A man is a candidate for watchful waiting if: his PSA density is less than 15 percent of the total weight of his prostate gland; no more than two samples of tissue show any evidence of cancer; less than 50 percent of any single sample contains cancer cells; and the cancer cells are deemed to be slow-moving.
The Foundation for Informed Medical Decision Making
A nonprofit medical education and research foundation based in Hanover, New Hampshire, which has produced videos on a variety of health topics including prostate disease. The videos are $49.95 plus $6.05 shipping and handling.
Us Too
A nonprofit support group organization for prostate cancer patients. Call 800-80-USTOO.




