One in 20 Americans will get cancer of the colon or rectum in his or her lifetime. In fact, colorectal cancer is the second most frequently diagnosed cancer in the United States. Although the disease strikes men and women in almost equal numbers, men are more likely to die of it.
In 1993 alone, colorectal cancer claimed the lives of 28,800 American men, making it the third deadliest cancer for men after that of the lung and prostate. Whereas the mortality rate for women has dropped by 30 percent over the last 30 years, the rate for men decreased by only 7 percent for the same period! The reason for this wide discrepancy is largely unknown, but delayed detection in men may be partially to blame.
That may in fact be the most important point to remember about colorectal cancer: One of the most serious cancers, it is also one of the most curable, when caught early. The overall cure rate is about 50 percent, but odds increase dramatically to more than 95 percent if the cancer is detected before it has had a chance to penetrate the colon walls or spread to nearby lymph nodes.
The incidence of colorectal cancer is much greater in industrialized countries, suggesting that environmental factors may contribute to its development. The most important of these is diet. There is a very strong correlation between the high-fat, low-fiber diet common in the Western world and the high incidence of colorectal cancer.
Age is another factor. As a person ages, his or her risk of getting colorectal cancer increases as well. The incidence of the disease rises after the age of 40, with more than 94 percent of cases occurring after age 50. The average age at diagnosis is 62.
Your family and personal health histories are also very important in evaluating your risk of colorectal cancer. The following factors should be discussed with your doctor to determine whether you should begin screening for colorectal cancer earlier or be tested more frequently than generally recommended:
| Estimated Incidence in Men (Total: 76,811) | |
| Age | Incidence |
| 0-14 | 0 |
| 15-24 | 65 |
| 25-34 | 456 |
| 35-44 | 1,873 |
| 45-54 | 5,823 |
| 55-64 | 14,128 |
| 65-74 | 26,115 |
| 75-84 | 22,234 |
| 85+ | 6,117 |
- A family propensity toward uterine, breast or colon cancer. The risk is greater if the cancer occurred in close relatives like parents, children or siblings. In fact, about 15 percent of all colorectal cancer patients have a family history of colorectal cancer in a close relative.
- Having multiple, small, tumor-like growths in the colon. These growths, known as polyps, which usually form in the colon or rectum during puberty, are a precursor to cancer. Their cells have a tendency to undergo malignant change, and cancer generally develops in all parts of the colon within about 15 years. Since doctors believe most colon and rectal cancers begin as polyps, it’s best to detect and remove these as soon as possible. A hereditary condition, known as familial polyposis, characterized by hundreds or thousands of these polyps, accounts for a very small percent of all colorectal cancer cases.
- Inflammatory Bowel Diseases, such as chronic ulcerative colitis and Crohn’s disease. These conditions cause inflammation of the lining and wall of the bowel. Scientists believe that colorectal cancer may result from cell overgrowth when new cells are generated to replace the diseased tissue.
- Having been treated for colorectal cancer or polyps in the past.
There are several ways you can help lower your risk of colorectal cancer. Here are some of the most important.
- Diet. A low-fat, high-fiber diet seems to reduce the risk of colorectal cancer by speeding the elimination of wastes from the body. This minimizes the amount of time the bowels are exposed to any carcinogens (cancer causing elements) that may be in feces. Researchers at the Harvard School of Public Health found that men who ate more fiber and less fat were 3.6 times less likely to develop intestinal polyps than those who ate high-fat, low-fiber foods. How much fiber should you get? The National Cancer Institute (NCI) recommends 20 to 30 grams of fiber a day, twice as much as the average adult now consumes.
Insoluble fiber is the type that matters most. Good sources: Whole-grain breads, cereals and pastas, beans, brown rice, and plenty of fruits and vegetables–at least five servings a day. Limit fat to 30 percent of daily caloric intake, with no more than 10 percent coming from saturated fats like butter and coconut and palm oils.
New research suggests that calcium and folic acid may contribute to the prevention of colorectal cancer as well. Good sources of calcium include skim or low-fat milk and dairy products, broccoli, kale, and salmon and sardines with bones. Folic acid can be found in fortified cereals, dark green leafy vegetables, some nuts and seeds, and dried beans.
- Smoking. Recent studies at the Harvard School of Public Health and Brigham and Women’s Hospital in Boston provide the strongest evidence to date linking cigarette smoking to colon cancer. In addition, the studies found that unlike with heart disease and lung cancer, in which quitting can reverse risk, early smoking (through your twenties) increases your lifetime risk of colorectal cancer. But remember that the longer you smoke, the greater your risk, so it’s never too late to stop.
- Exercise. Studies suggest that regular physical activity cuts colon cancer risk practically in half (there is no evidence of a similar protection against rectal cancer), possibly by speeding up the digestive process and shortening the bowels’ exposure to carcinogens. But researchers point out that the beneficial effects of exercise may be due to other aspects of a healthy lifestyle common in people concerned about fitness.
- Aspirin. Preliminary research points to a protective effect of aspirin against colorectal cancer. But the research is still inconclusive and other risks associated with aspirin (such as erosion of the stomach lining and tumors of the urinary tract) need to be explored before regular use is recommended.
Since colorectal cancer is one of the more treatable cancers, it’s especially important to catch it early, when chances of cure are greatest. If you experience any of the symptoms listed below for more than two weeks, see your doctor. They could indicate a non-cancerous intestinal disorder, such as an ulcer or hemorrhoids, or could be a sign of cancer. Only your doctor can tell for sure.
- Diarrhea or constipation
- Rectal bleeding or blood in the stool
- Stools that are smaller in width than usual
- General stomach discomfort (bloating, fullness, cramps)
- Frequent gas pains
- A constant feeling of having to go to the bathroom (tenesmus)
- Unexplained weight loss
- Constant tiredness
- Unexplained anemia
When colorectal cancer is detected at an early localized stage, the five-year survival rate is 95 percent for colon cancer and 85 percent for rectal cancer. Once the cancer has spread to regional lymph nodes or other organs, those numbers drop to 61 percent and 51 percent respectively. The survival rate for people whose tumors have spread to other parts of the body is less than 7 percent.
Screening, therefore, is clearly important, but there is a great deal of controversy over which methods are best and most cost-effective.
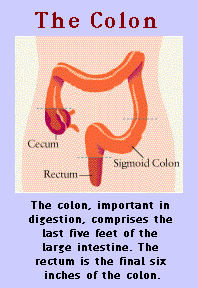
The colon, important in digestion, comprises the last five feet of the large intestine. The rectum is the final six inches of the colon.
- Digital rectal exam and fecal occult blood test. These tests are the most commonly performed. Both are completely safe and painless. In the digital rectal exam, the doctor inserts a gloved finger into the rectum to check for abnormalities on its walls. But this exam, which can be done in the doctor’s office, is limited to the rectum and cannot detect abnormalities in the colon. The fecal occult blood test checks for blood in the stool. Last year, a University of Minnesota trial found that such annual screening reduced colorectal cancer mortality by one third. But the test is not foolproof since bleeding does not always accompany colon cancer and blood in the stool can be caused by any number of other non-cancerous conditions.
- Flexible Sygmoidoscopy. The doctor uses an endoscope, a thin, flexible optical device, to examine the lining of the sigmoid, the last two feet of the colon, where more than 40 percent of colon cancers occur. This test is highly accurate, but it has a one-in-2,500 risk of perforating the colon wall. Another draw-back: A sigmoidoscopy does not examine the entire colon.
- Colon x-ray (sometimes called a barium enema). This procedure allows the doctor to check the entire colon by releasing a chalky liquid (barium) into the colon and taking an x-ray of the colon wall.
- Colonoscopy. This test often combines detection and treatment. Using a long, flexible endoscope, the doctor can look at the lining of the colon and remove most polyps and small cancers at the time of the exam. One problem: A colonoscopy may not reach the cecum, the pouch of tissue that joins the large and small intestines, where 20 percent of cancers occur. Sometimes a biopsy, in which the doctor removes a sample of tissue to determine if there are any malignant cells, is performed. A colonoscopy carries with it a one-in-500 risk of perforation.
- Future Forecast. The most exciting news in colon cancer detection may be the discovery of two genes which account for a large percentage of cases of hereditary colon cancer–up to 95 percent–as well as many cancers that don’t appear to have a family connection. Scientists expect to develop a blood test to screen for these genes within a year, making early detection and intervention easier for those with a family history of colon cancer. An accurate blood test for the general population is further away.
The American Cancer Society recommends men and women get an annual digital rectal exam after age 40, an annual fecal occult blood test after age 50, and a sigmoidoscopy (preferably flexible) every three to five years after age 50. If any of these tests indicate a problem, other exams, such as a colonoscopy and a colon x-ray may be needed. Your internist can do a digital rectal exam and fecal occult blood test during your annual physical. Some internists can also perform the other tests. If your doctor can’t, you’ll need to go to a gastroenterologist.
Unlike with other cancerous tumors, in the case of colon cancer the size of the tumor has little influence on prognosis and method of treatment. Unless the cancer is small enough to be removed by colonoscopy, surgery, or colectomy, is the primary therapy. The extent of the colon removed, and the use of additional therapy depends on the degree of the tumor’s penetration into the bowel wall, the involvement of regional lymph nodes and how far the cancer has spread.
- Surgery. In surgery the tumor and any affected surrounding tissue, including lymph nodes, are removed through an abdominal incision. The tissue is examined to make sure there’s a large enough margin of benign tissue surrounding the tumor to help ensure that no cancer has been left behind. Since the surgeon decides how much tissue needs to be removed, his or her experience with surgery for colon and rectal cancer impacts the surgery’s success.
Once the cancerous tissue is removed, the ends of the remaining colon or rectum are reconnected using sutures or staples (which don’t need to be removed). If the cancer is situated very low in the rectum, and there isn’t enough tissue left to put back together, a colostomy is performed. This involves the creation of an abdominal opening for the elimination of body wastes into a bag. Although fairly common at one time, thanks to modern surgical techniques, less than 3 percent of patients now require a colostomy. Another surgical procedure, called laparoscopy, is now starting to be used, too. Unlike traditional surgery, it requires just four or five small puncture wounds in the abdominal wall, through which the surgeon inserts instruments which allow him or her to see and remove the malignant area. This removal requires a far smaller incision than that required in traditional surgery. But the procedure is still controversial, because though it appears to be as effective as open surgery with a shorter recovery time, more trials and at least five to eight more years are needed to assess long term success.
After surgery, most people will experience erratic bowel movements: constipation one day, diarrhea the next. This should not be cause for concern unless the diarrhea is excessive or constipation persists for longer than two days. A carcinoembryonic antigen (CEA) blood test is commonly used to monitor patients for cancer recurrence. The average cost of the test is below $100, but its effectiveness has come under fire from researchers at several medical institutions, including the Mayo Clinic in Rochester, Minnesota. A study of more than 1,200 colon cancer patients found that only 2.3 percent of patients who had second operations based on CEA test results were alive and cancer-free a year later, compared to 2 percent of those who had not been tested. Researchers also found that the test missed many recurrences and often resulted in false positives, requiring additional, expensive tests and even surgery in some cases to rule out cancer.
- Chemotherapy. This therapy uses drugs to kill cancer cells. Until recently there was no evidence of its effectiveness in the treatment of colorectal cancer and even now it is mostly used as adjuvant therapy.
Candidates for chemotherapy are people with cancer that has spread to the lymph nodes. Chemotherapy is usually begun about one month after surgery and continued for six to 12 months. The type of chemotherapy used for colorectal cancer is usually less traumatic to the system than that used to treat other types of cancer. Chemotherapy may also be recommended when the cancer has spread too far for surgery to be effective, and in conjunction with radiotherapy for patients with rectal cancer. Radiotherapy, or radiation, uses x-rays or gamma rays to stop cancer cells from proliferating. Doctors are experimenting with radiation therapy during surgery, too, after the surgeon has removed as much of the malignant tissue as possible. Although intra-operative radiation appears to improve post-surgical survival rates, its long-term effectiveness is still unknown.
In the fight against colorectal cancer, early detection is key to increased survival rates. Men in particular need to be more diligent about regular screenings for the disease. The exams you undergo now could save your life later.
Colon Cancer Survival Rates
| Cancer Stage | Definition | Survival Rate |
| 0 | Cancer has not penetrated bowel | 95 to 100% |
| 1 | Cancer has penetrated but is limited to, the bowel wall | 75 to 100% |
| 2 | Cancer has spread to tissue outside the bowel walls | 50 to 75% |
| 3 | Cancer has spread to local lymph nodes | 30 to 50% |
| 4 | Cancer has spread to other organs | 10% |
Our thanks to Jacques Van Dam, M.D., Ph.D., Director of Endoscopic Gastrointestinal Oncology and Associate Director of Gastrointestinal Endoscopy, Brigham and Women’s Hospital, Boston, MA, and Samuel Labow, M.D., Associate Clinical Professor of Surgery, Cornell University, Great Neck, NY, for reviewing this article.
Cancer Information Service
This nationwide service of the National Cancer Institute is set up to answer questions from the public. The booklet Cancer of the Colon and Rectum is available free of charge.
800-4-cancer
American Cancer Society
Among the variety of services the ACS offers is a support program for people with colostomies. Contact your local chapter for more information.
800.227.2345




