Your doctor tells you that you’re pregnant. If you’re like most women, you go from unrestrained euphoria to high anxiety in the span of a few minutes or less. Hundreds of questions and concerns take hold of your mind: What should I eat or not eat? Are there things you can do to help your baby develop properly? What should you expect once the big day arrives?
Learning about pregnancy and good prenatal care (including proper nutrition and exercise) can reduce or eliminate serious risks for both mother and child. Complications during labor can be averted. And risk factors like low birth weight (under five and a half pounds), which is associated with an estimated 300 percent increase in other birth defects, can often be prevented.
Another good reason to learn about pregnancy: Education provides options. It makes choices appear where superstition, dictates and customs previously ruled.
Lastly, learning about pregnancy can help alleviate the fear of the unknown that often accompanies a woman’s discovery that she is pregnant. We are all frightened of things we do not understand. Once understood, pregnancy can not only be better managed, it can actually be enjoyed.
A Good Diet:
Building Block For Infant Health
Some people believe that the fetus will get all the nutrients it needs from the mother’s body. This is both true and untrue at the same time. The foods a pregnant woman eats are the foods her baby eats. Click here to see what the weight you gain breaks down to.
The special nutritional needs of the growing baby make it particularly important for the mother’s diet to be nutritionally sound. If, for example, you’re not eating enough calcium-rich foods, the baby will sap your own stores of the mineral to get the amount he or she needs.
If you’re lacking certain nutrients, the baby will, too. Through her diet and the care she takes, a mother-to-be gives her child a well-nourished body.
Diet Do’s and Don’ts
1. Eat a wide variety of foods. A well-balanced diet means eating a variety of good foods like fruits, vegetables and grains, as well as dairy products (milk and cheeses) and proteins (meats, fish, eggs, nuts and beans). It is important to eat foods from each of these groups every day to ensure that the baby gets all the nutrients he or she needs in order to develop properly.
Since it’s difficult for many women even when they are not pregnant to get the Recommended Daily Allowance of essential vitamins and minerals, ask your doctor about taking a prenatal supplement. Of particular importance: Folic acid, found in dark green leafy vegetables and proven to prevent neural tube defects. It is very difficult to get enough folic acid from diet alone, so experts are now urging women who plan to become pregnant as well as those in the first months of pregnancy to take a supplement.
2. Avoid added sugars and fatty or fried foods, and eat whole grains only. Foods lose many important nutrients when they are processed.
3. Eat smaller meals more frequently. During pregnancy, your stomach and intestines are pushed up and back by your expanding uterus and the growing baby. You may find that you no longer have room for large meals. Smaller meals, eaten more frequently, will leave you feeling far more comfortable since they are more easily digested.
By nibbling throughout the day, you can also help forestall nausea, a common complaint of pregnancy. Morning sickness can sometimes be prevented by eating a light snack in the middle of the night or a little something, like crackers, before getting out of bed in the morning.
4. Drink plenty of fluids, especially water and juices. Doctors recommend pregnant women drink at least eight glasses of water each day. More fluids are needed during pregnancy in order to support the increase in the mother’s blood volume and maintain the amniotic fluid surrounding the baby. Increased fluid intake also helps prevent constipation. Avoid caffeinated drinks like coffees, teas and colas. And stay away from all alcoholic beverages.
Danger: Alcohol, Drugs, Smoking And Your Baby
One out of every 14 babies born in the U.S. in 1990 was born with a birth defect, according to the March of Dimes. Many of those birth defects could have been prevented. There is no better time than when you are pregnant to quit or cut down on harmful habits. Don’t worry about past uses; just make sure they are your last. Here are some important points to keep in mind:
- Wine, beer and hard liquor can cause serious harm to a growing fetus. When you drink, your baby drinks. Since nobody knows how much is too much, it’s best not to drink any alcohol during pregnancy.
- Illegal drugs, such as marijuana, cocaine, crack, heroin and PCP have all been shown to pose serious health risks to both the pregnant woman and her unborn child. Even legal drugs can have harmful effects. So avoid all medications except those prescribed by your doctor. This includes over the counter drugs.
- Research has shown that smoking during pregnancy raises the risk of premature delivery, low birthweight and intellectual deficiencies in childhood. Nicotine constricts uterine blood vessels, decreasing the amount of nutrients and oxygen the fetus receives.
The American Lung Association’s (ALA) quit-smoking program “Freedom From Smoking for You and Your Baby” is specially designed for pregnant women. To buy the step-by-step manual and audio tape call 800-LUNG-USA.
What is Prenatal Care
and Why is it so Important?
Prenatal care entails regular visits to a doctor, midwife or clinic throughout pregnancy. These checkups help safeguard your health as well as the health and well-being of your baby.
Regular prenatal visits help your doctor or midwife identify and treat or prevent problems such as anemia (low levels of iron and oxygen in the blood), gestational diabetes (diabetes which only occurs during pregnancy) and pre-eclampsia (a potentially dangerous condition signaled by abnormal swelling, high blood pressure and protein in the urine). These and other conditions are often easily corrected when discovered early, but left untreated, they can threaten your health as well as the health and even the life of your baby. The schedule of your prenatal visits will vary, depending on your practitioner, but usually will include:
1. An overall physical exam. This exam should be scheduled within a week or two of discovering you’re pregnant. Your practitioner will confirm your pregnancy, determine the state of your general health and pinpoint any possible problems that need treatment or monitoring.
2. Regular monthly checkups for the 1st through the 7th month. Your doctor will listen to the baby’s heartbeat and measure your uterus (from the outside) to ensure that your baby is growing normally. He or she will determine whether you are gaining enough weight and will check your blood pressure, test your blood (for anemia) and urine (for sugar and protein), and examine your hands and feet for signs of abnormal swelling (edema). Alert your doctor to any physical problems you might be having. Write down any questions before your checkup so you won’t forget to ask them.
3. Regular checkups every 2 weeks in the 8th month, once a week in the 9th month, until the baby is born. These will be similar to earlier exams except that your practitioner will also carefully examine the size and position of the baby as well as check your cervix to see if it is softening or thinning out in preparation for birth. Some practitioners refer to the cervix as “green” when it is firm and “ripe” when it is soft. A soft, ripe cervix means the baby will be born soon!
Tests You Can Expect During Pregnancy
Experts agree that a woman should begin to undergo routine screening tests either before conception or at her first prenatal visit. These tests alert doctors to potential problems and provide a basis for comparison as the pregnancy progresses. Here are some straightforward answers to questions about the most common tests during pregnancy, their risks and why they are necessary.
First Trimester Tests
- Tests for glucose, protein and blood in the urine to detect problems such as impaired kidney function and diabetes
- A cervical culture for gonorrhea and chlamydia
- Blood tests to determine blood type and Rh type (to test for Rh incompatibility) and to check for anemia
- Tests for rubella and toxoplasmosis (a parasitic infection) and hepatitis B
- Chorionic Villus Sampling (CVScan detect defects in the fetus as early as the ninth week of pregnancy. The problem: The possible risk the test poses. Studies conducted in 1992 yielded conflicting results concerning the safety of CVS. Researchers at Michael Reese-Humana Hospital in Chicago found a higher incidence of limb defects in babies born to women who had undergone CVS. However, most other studies, including a later one conducted by researchers at Jefferson Medical College in Philadelphia, found CVS to be safe. Before having CVS, discuss the benefits and risks of the procedure with your doctor, and don’t be afraid to request a second opinion.
Second Trimester Tests
- Ultrasound (or sonography) is a procedure that can be performed from the fifth week of pregnancy up until delivery, but it is generally done after the sixteenth week. The test uses sound waves to produce a picture of the fetus (sonogram) without the danger of x-rays. Most ultrasound machines have a TV-like screen that provides parents-to-be a unique opportunity to see their baby. Often they can even get a copy of the sonogram to show to family, friends and their child in later years.
If performed early, ultrasound it can be used to date a pregnancy. Later, it can be used to identify possible causes of a problem such as vaginal bleeding, determine the condition of the placenta, diagnose a multiple pregnancy, determine whether the baby is growing properly and verify breech presentation or another uncommon fetal or cord position prior to delivery.
Although in 25 years of clinical use and study, no harmful effects have been associated with ultrasound, the American College of Obstetricians and Gynecologists (ACOG) still recommends the procedure be performed only when necessary – not on a routine screening basis. Many obstetricians provide ultrasound services in their offices.
- Alpha-Fetoprotein (AFP) Screening, performed between the fifteenth and eighteenth week of pregnancy, analyzes the mother’s blood to detect the possibility of abnormalities in the baby’s brain or spinal cord or a chromosomal disorder such as Down’s syndrome. The problem with the AFP test is the high number of false positives it produces. If you have an AFP screen, remember, it is only a screening test. Any abnormal results require further testing to confirm a problem. Because the test can detect possibly serious illnesses and poses no danger to the mother or the fetus, experts recommend AFP screening for all pregnant women.
- Amniocentesis, usually performed between the fourteenth and eighteenth week of pregnancy, is a diagnostic test that can identify a number of fetal problems, including Down’s syndrome and the possibility of Tay-Sachs disease or sickle-cell anemia. Since Down’s syndrome is more common in babies born to older women, amniocentesis is usually recommended for all women over age 35.
How it works: the doctor inserts a slender needle through the abdomen and into the amniotic sac and extracts fluid for examination. Through chromosome analysis the test can also reveal the sex of the fetus.
Third Trimester Tests
A number of the tests performed earlier, such as those for glucose tolerance, are repeated or updated in the third trimester. If your doctor suspects a problem, he or she may also recommend additional testing.
It’s Time: The Drama of Birth
For most new parents childbirth is not a sequence of orderly stages, but rather a blur of new physical and emotional experiences. Emotions seesaw from excitement to apprehension. The more you learn about the process of labor and delivery, the better prepared you’ll be. Here’s a preview of what to expect.
Click here for a summary of the different types of child birth classes usually available.
Labor: What is it?
Make no mistake, as its name implies, labor is hard work. During labor, the muscles of your uterus contract (tighten) and relax at increasingly shorter intervals. These contractions cause the cervix, the entrance of the uterus, to dilate (open). Once the cervix is fully dilated, the contractions help move the baby through the birth canal (vagina).
First Stage of Labor
The first and longest stage of labor is fortunately also the least intense. During this period, which can last many hours, the cervix begins to dilate. Contractions at this stage are usually mild to moderately strong. In most cases there’s no need to be at the hospital until contractions increase in intensity and come about five minutes apart.
What will happen at the hospital? Once you’ve been admitted to the hospital, your nurse or physician will check your blood pressure, pulse, respiration and temperature, and will listen to your heart and lungs. Your doctor will feel your abdomen to assess the weight and position of the baby, and may do a vaginal examination to determine how much the cervix has dilated. By this time, your cervix probably will have dilated between four and seven centimeters.
Your doctor may also check your baby’s heartbeat with a fetal stethoscope or an external fetal monitor. The monitor is strapped around the mother’s abdomen to record the baby’s heartbeat and the pressure of labor contractions. If fetal distress is suspected, the doctor may opt for internal fetal monitoring, in which an electrode is inserted through the cervix and attached to the baby’s scalp.
Easing Labor Pains. Everyone responds differently to discomfort and pain. To combat the pain of labor and delivery, you may find that all you need are your relaxation techniques and the support of the people around you. Or you may feel you need pain relievers.
Although many women believe natural childbirth (in which no drugs are used) is a wonderful experience, you should not feel guilty if you can’t or don’t want to go through labor without pain relievers. There are a number of medications from which to choose. Some, such as Demerol, are injected. Others, such as Phenergan, which can help reduce anxiety and nausea, are taken orally. An epidural, which is a regional anesthetic, blocks sensation from the waist down. Talk to your doctor about each drug’s pros and cons to determine which is right for you.
Transition. This refers to the final three centimeters of dilation, to a full 10 centimeters. It is the most exhausting and demanding phase of labor. Your coach’s support and reassurance will be especially welcome at this time.
The Second Stage of Labor:
Here Comes the Baby!
Active labor, or the actual BIRTH of the baby usually lasts about an hour or two for first-time mothers, 30 minutes for women who’ve given birth before. In pushing, the woman uses her abdominal muscles to move the baby down the birth canal. Between contractions, when both the uterine and abdominal muscles are relaxed, the baby usually slips back a little. Pushing is a 2 down, 1 back process until the baby’s head starts to crown-is visible in the vagina.
If necessary, your doctor will perform an episiotomy-an incision that widens the vaginal opening to prevent tearing or to speed delivery-before crowning. A local anesthetic may be administered to numb the area before the cut is made. Stitches will dissolve by themselves a few days after the birth. Whether you need an episiotomy will probably depend upon your skin’s elasticity and the baby’s size. Find out how your doctor feels about episiotomies before labor begins.
If any complications arise that make vaginal birth dangerous for either mother or child, the doctor may decide to perform a cesarean section.
Third Stage Of Labor:
The Afterbirth
This is the shortest stage of labor, usually lasting less than 30 minutes. After the baby is born, you will continue to have mild contractions which will help push out the afterbirth (placenta, umbilical cord, and amnion).
While your baby will undergo several routine procedures, including weight and height measurements, foot printing, and the administration of silver nitrate eye drops to prevent infection. A nurse will observe the baby’s heart rate, breathing, muscle tone, reflexes and color at one and five minutes after delivery and give him or her an Apgar (Appearance, Pulse, Grimace, Activity, Respiration) score. These post birth examinations assess the baby’s condition on a scale of zero to 10. Vigorous babies score 7 or higher.
Our thanks to Vrunda Patel, M.D., Princeton Medical Center, Princeton, N.J, for reviewing this article.
Cesarean Section: The Controversial Cut
In 1984, Cesarean section, often called a C-section, in which the baby is taken from the womb through an abdominal incision, became the most common operation in the United States. In fact, nearly one out of every four babies in this country – a full 23.5 percent – is delivered via C-section. Critics claim that C-sections as one of the most over-performed procedures in the country, needlessly risky to the mother and providing no clear without benefit to the baby. But the fact is a Cesarean is called for when a vaginal delivery is thought to be dangerous for either mother or child. The mother is typically awake during a Cesarean, which is usually performed under regional anesthetic (such as an epidural) injected into the spine. The baby’s father can usually remain at her side. From first incision to delivery usually takes five to 10 minutes; closing the cut takes about 45 minutes. Women may feel greater physical discomfort after a Cesarean birth than after a vaginal birth and should refrain from strenuous activity for several weeks.
How Can You Know if a Cesarean is Really Necessary?
Here’s a look at the most common reasons for Cesarean sections:
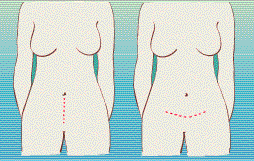
1. A previous Cesarean delivery. At 36 percent, repeat Cesareans are still the number one reason for Cesarean delivery. Up until very recently, doctors feared that the uterus of a woman who had a Cesarean would rupture during a subsequent vaginal labor. But the risk of that happening is actually very small, especially in the case of a low horizontal incision (see illustration). The good news: Many doctors now support Vaginal Birth After Cesarean (VBAC) if the mother and baby have no medical problems.
2. Dystocia-When the baby’s head is too big to pass through your pelvis or when labor does not progress. To help contractions along, try the relaxation methods you learned in your childbirth education classes and experiment with different birthing positions. Some physicians will try to give sluggish contractions a boost with oxytocin (a drug used to initiate or speed up labor) before resorting to a Cesarean.
3. Breech birth-When the baby’s feet or bottom appear first. The usual position of engagement is head-down. Many breech babies turn around by themselves; exercises may help. A caregiver may try to turn the baby before delivery starts. Although some caregivers will deliver a breech baby vaginally, most breech babies are delivered by C-section.
4. Fetal stress. This can occur if the baby is not getting enough oxygen. Possible signs of fetal stress: a change in the baby’s heart rate or a meconium stain, which occurs when the baby has a bowel movement in utero, turning the fluid around the baby from clear to green, yellow or brown. Your caregiver may want to monitor the baby more closely through internal electronic monitoring or take a fetal blood sample to determine the need for a Cesarean.
5. Maternal medical problems. Premature labor or a condition such as high blood pressure or diabetes may make a vaginal birth too risky to attempt.
Why Have C-Section Rates Increased So Dramatically?
- Technology. Advances in medical technology have enabled doctors to detect problems and safely deliver by Cesarean babies who would have otherwise died.
- High malpractice premiums. Malpractice suits against obstetricians have increased dramatically over the last decade. The legal liability associated with difficult vaginal deliveries in which something could go wrong may pressure doctors to perform C-sections more often than is medically necessary.
- “Once a C-section, always a C-section.” Cesareans may be self-perpetuating. Once a patient has had one C-section, many doctors will routinely perform a Cesarean with subsequent deliveries even when a vaginal birth is possible, despite the increased acceptance of VBACs.
National Statistics As the charts below show, after almost two decades of steady growth, the national C-section rate appears to be dropping. At the same time, the number of Vaginal Births After Cesarean (VBACs) is steadily rising.
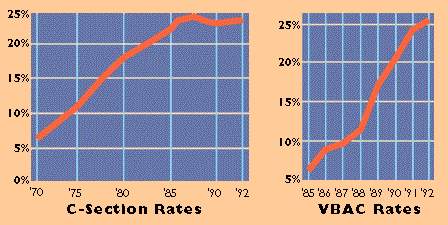
Source: National Center for Health Statistics, 1994
What is a VBAC?
Vaginal Birth After Cesarean involves a trial of labor which can result in either a vaginal birth or another C-section.
In 1988, ACOG issued guidelines in an attempt to curtail routine repeat C-sections. The guidelines advise doctors to give women who have previously given birth by C-section the opportunity to let labor progress naturally. In 1990, 20 percent of women who previously had a Cesarean gave birth vaginally. That’s up from 13 percent in 1988 and less than 4 percent in 1980.
What are the advantages of a VBAC?
1. Less risk. A vaginal birth usually results in fewer medical problems for both the mother and the baby than Cesarean .
2. Shorter recovery. Because there’s no surgery from which to recuperate, a woman generally feels better and can resume her everyday activities sooner after a vaginal delivery.
3. More involvement. Many women want to be actively involved in childbirth and a vaginal delivery allows for greater participation.
Are You a Candidate for VBAC?
There are a number of issues caregivers must consider when deciding if a woman can have a VBAC. Key factors that make a VBAC attempt possible:
- 1. Neither the mother nor the baby has any major medical problems.
- 2. The health of the mother and baby can be closely supervised during labor.
- 3. The uterine incision from the previous Cesarean is horizontal.
What to Ask Your Doctor About C-Sections
- Are you planning to deliver the baby by Cesarean? Why? Do I have any other alternatives?
- My first baby was delivered by C-section. Will you let me try a vaginal birth this time?
- If my labor doesn’t progress, will you try other procedures, like medication, before performing a C-section?
- If the fetal monitor indicates the baby is in distress, will other methods be used to confirm the monitor’s reading before a C-section is performed?
- Will the type of incision you make render me unable to attempt a vaginal delivery with my next child?
- Will the father be able to be present during the Cesarean and hold the baby immediately after the birth?
- Can the baby stay in the room with me after the birth?
- How long will I need to stay in the hospital?
- What physical discomfort and limitations can I expect following the surgery?
The Weighting Game
The weight you gain during your pregnancy helps your body nourish your growing baby and produce the milk you’ll need for breastfeeding. There’s no magic number when it comes to the amount of weight a woman should gain while she’s pregnant, but the average healthy woman gains between 25 and 35 pounds. Expect to gain about 10 pounds during the first 20 weeks and about one pound per week for the remainder of your pregnancy. However, don’t take the need to gain weight as a license to binge on junk food. Remember, the important thing is not how much weight you gain, but the kinds of foods you’re eating to gain it.
What is All That Weight?
7 Pounds: Maternal stores (fat, protein and other nutrients)
4 pounds: Increased fluid volume
4 pounds: Increased blood volume
2 pounds: Breast enlargement
2 pounds: Uterus
6-8 pounds: Baby
Total: 25-27 pounds
Childbirth Classes 101
The more prepared you are for labor and delivery, the better. That’s why many couples take childbirth education classes before the big day. These classes offer much needed moral support for parents-to-be.
There are several approaches and philosophies from which you can choose. Many classes combine elements of various methods. Lamaze, the most commonly used method, centers on education and relaxation techniques which include a series of breathing exercises to be used during contractions. Bradley, another popular philosophy, emphasizes the father’s role as labor coach. When shopping around for a class, ask your doctor or health care practitioner for recommendations and visit prospective classes to determine what’s right for you. See Health Pages’ Hospital Maternity Services chart for information on local childbirth classes.




