Your heart is the engine that keeps your body going. Every day this vital organ beats about 100,000 times, pumping the equivalent of 2,000 gallons of blood. Your heart works hard for you, and, in turn, there’s a lot you can do to keep it in top form.
What is the number one killer in America? If you guessed cancer, you’re wrong. Cardiovascular disease holds that deadly distinction for both men and women. As the chart below illustrates, diseases of the heart and circulatory system claimed 926,079 victims in 1990-that’s 420,757 more than cancer did. In fact, someone dies from some form of cardiovascular disease every 34 seconds.
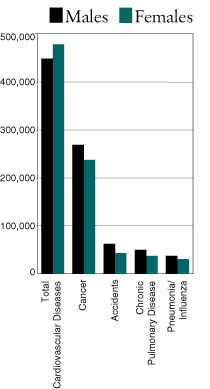
Despite these staggering numbers, there is good news too. Death rates from heart attack, stroke and other cardiovascular diseases are declining due to advances in medical treatment and healthier lifestyles. Still, there is no room for complacency particularly because the following measures may prevent many of these deaths:
- Lower high blood pressure
- Stop smoking
- Control blood cholesterol
- Stay physically active
- Know the warning signs of cardiovascular disease
Understanding how this killer works is essential. That is why Health Pages has dedicated this Special Report to help explain everything you need to know to keep your heart healthy.
How Your Heart Works
The heart is a strong muscle that’s a little larger than your fist. It continuously pumps oxygen- and nutrient-rich blood throughout the circulatory system, which also includes the lungs, arteries, veins and other blood vessels. The heart has four chambers, and blood is pumped through them each time the heart expands and contracts (beats).
In order for the heart to function properly, the four chambers must beat in an organized manner. This rhythm is governed by an electrical impulse that starts in a small bundle of highly specialized cells-the heart’s natural pacemaker-located in the right atrium (see illustration below). Anything that interferes with the heart’s ability to pump blood through the body spells trouble. The American Heart Association (AHA) estimates that 56,450,000 Americans have one or more forms of cardiovascular disease.
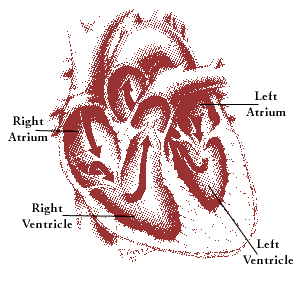
The heart’s natural pacemaker, located in the right atrium,
regulates the flow of blood by controlling the
synchronized beating of the four chambers
Risk Factors for Heart Disease
There are several factors that can disrupt the cardiovascular system, thus increasing the risk of heart disease. These can be divided into two groups: risk factors that can’t be changed and those that can.
1) Risk Factors That Can’t Be Changed
Heredity. Children of parents with cardiovascular disease are more likely to develop it themselves.
Race. African-Americans have moderate high blood pressure twice as often as whites and severe hypertension three times as often, so their risk of heart disease is greater.
Age. About four out of five people who die of heart attack are age 65 or older. In this age group, women who have heart attacks are twice as likely as men to die from them within a few weeks.
Diabetes. More than 80 percent of people with diabetes die of some form of cardiovascular disease. Part of the reason for this is that diabetes boosts blood levels of cholesterol and triglycerides (fatty substances that are made in the body or that come from food). To control diabetes, a doctor may suggest changes in eating habits, weight control and exercise programs. Drugs may also be prescribed to keep the disease in check (see our article The Sweet Truth About Diabetes).
| Myth: If I develop a problem, angioplasty or surgery will fix it. Fact: These procedures are a means of last resort, providing temporary management in a critical situation. The key to a healthy heart is prevention. |
2) Risk Factors That Can Be Changed
Smoking. Smokers’ risk of heart attack is more than twice that of nonsmokers, and smoking is the biggest risk factor for sudden cardiac death. In fact, smokers who have a heart attack are more likely to die within an hour than are nonsmokers.
The evidence is also mounting against chronic exposure to second-hand smoke. The risk of death due to heart disease is increased by about 30 percent among those exposed to environmental tobacco smoke at home. And that threat could be much higher among those exposed to smoke in the workplace, where even higher levels may be present.
The good news: When people stop smoking, regardless of how long or how much they’ve smoked, their risk of heart disease rapidly declines. Three years after quitting, the risk of death from heart disease and stroke for people who smoked a pack a day or less is almost the same as for people who never smoked. But it is important to stop smoking before the signs of heart disease appear.
High Blood Cholesterol. The risk of coronary heart disease rises as blood cholesterol levels increase. According to the AHA, blood cholesterol levels should be measured at least once every five years in healthy adults over 20. A certain amount of cholesterol in the body is necessary, but the liver produces enough of it to meet these needs. That’s why it’s important to control your dietary intake of saturated fat and cholesterol, which can raise blood cholesterol levels (see Eating Plan Tips).
High Blood Pressure (hypertension). This risk factor increases the heart’s workload, causing it to enlarge and weaken over time. High blood pressure is called a “silent killer” because it has no specific symptoms or early warning signs. As a rule, blood pressure increases with age. Eating a proper diet, losing weight, exercising regularly, restricting sodium intake, and taking medication may all be prescribed to keep blood pressure within healthy limits (see Heart-Saving Tests).
Physical Inactivity. Lack of exercise can lead to excess weight and increased blood cholesterol levels. Regular aerobic exercise (jogging, swimming, tennis, etc.) plays a significant role in preventing heart and blood vessel disease. Even modest levels of low-intensity physical activity, such as walking, gardening and dancing, are beneficial if done regularly and for adequate periods of time (see Exercising Your Heart).
Obesity. People who are more than 30 percent over their ideal body weight are more likely to develop heart disease, even with no other risk factors. That’s because extra weight puts a strain on the heart, increases blood pressure and cholesterol, and can lead to diabetes.
According to the AHA, recent evidence suggests that the distribution of fat on the body may affect the risk of coronary heart disease as well. A man’s waist measurement should not exceed his hip measurement, and a woman’s waist measurement should not be more than 80 percent of her hip measurement. To figure out your waist/hip ratio, divide your waist measurement by your hip measurement. Optimally, the result should be no greater than 1.0 for men and 0.8 for women.
| Myth: As long as I watch my cholesterol, I can eat whatever I want. Fact: Cholesterol is not the only dietary enemy to your heart. A diet high in calories, fat and sodium also increases your risk of heart disease. |

MOST COMMON CARDIOVASCULAR DISEASES
Cardiovascular disease (CVD) is any abnormal condition of the heart and blood vessels. The AHA estimates that over 56 million Americans suffer from one or more types of cardiovascular disease. The most common of these are high blood pressure, coronary heart disease and stroke. In this section, we explain what each of these entails and how they can be treated
High Blood Pressure
When your heart beats, it pumps blood through large blood vessels called arteries, which conduct blood from your heart to other parts of your body. As your blood is pumped through your arteries, it pushes against the artery walls. This force against the artery walls is called blood pressure.
Blood pressure is what makes your blood circulate, but it never stays the same; it constantly adjusts to your body’s needs. For instance, your blood pressure rises when you exercise or are excited and drops when you rest or sleep. Blood pressure only poses a problem when it is regularly above an acceptable range (see Heart-Saving Tests).
What Is High Blood Pressure?
Healthy arteries are muscular and elastic; they stretch when the heart pumps blood through them. However, blood flow is hampered if the arteries become too narrow. Consequently, your blood pressure rises and your heart has to work harder to get the blood through.
In about 90 percent of cases of high blood pressure, the disorder has no known cause. This is called essential or primary high blood pressure. When hypertension is a symptom of an underlying problem, such as a kidney abnormality or heart defect, it is called secondary high blood pressure.
Certain factors boost a person’s chance of developing hypertension, including all of those listed for heart disease (except diabetes) plus:
- A sensitivity to sodium. In some people, eating too much salt can lead to high blood pressure. That’s why doctor’s must put certain hypertensive patients on strict sodium-restricted diets.
- Alcohol Consumption. Studies have shown that heavy, regular consumption of alcohol can increase blood pressure dramatically.
- Oral Contraceptives. Women who take oral contraceptives may develop high blood pressure. This risk increases several times if a woman also smokes.
| Myth: If I am not tense, I can’t have hyper-tension. Fact: The tension in hypertension refers to mechanical forces in the walls of arteries, not to emotional tension. |
How Does High Blood Pressure Affect Me?
Uncontrolled high blood pressure adds to the workload of your heart and arteries, making it more difficult for them to meet the body’s demands.
Arteries harden and become less elastic with age in everyone, but high blood pressure tends to speed up this process. High blood pressure also increases the risk of stroke and can damage your kidneys.
Treating High Blood Pressure
Treatment for high blood pressure usually includes some combination of diet, exercise and medication. If you are overweight, a healthy diet and exercise can help you lose the extra pounds, which often lowers blood pressure automatically. A low-salt diet is also often recommended to lower blood pressure. In addition, there are many medications available to reduce high blood pressure. Some help rid the body of excess fluid and sodium (salt can often increase the amount of water the body normally retains). Others open up narrowed blood vessels. Still other types of drugs stop blood vessels from constricting.
Coronary Heart Disease
Coronary heart disease (sometimes referred to as coronary artery disease) is a general term for both heart attack and angina. A heart attack occurs when the life-giving blood supply to part of the heart muscle is severely reduced or stopped and heart tissue is destroyed by a lack of oxygen. Such an event usually happens when a blood clot blocks blood flow in a coronary artery that is already narrowed by fatty deposits (atherosclerosis), a major cause of cardiovascular disease.
What is Atherosclerosis?

Atherosclerosis comes from the Greek word athero (gruel or paste) and sclerosis (hardness). As this implies, it is characterized by deposits of fatty substances, such as cholesterol, and other materials hardening on the inner lining of an artery. The resulting buildup is called plaque and it can partially or totally interfere with blood flow through an artery.
What is Angina?
Angina, characterized by chest pain, is a symptom of a condition called myocardial ischemia, which occurs when the heart muscle isn’t getting as much blood as it needs to function. Angina can occur when blood circulation to the heart is enough for normal needs but not enough for physical exertion or emotional excitement. Angina can be a warning sign of heart attack.
How Is Coronary Heart Disease Treated?
Medications. Some drugs cause blood vessels to relax, thereby widening them and improving blood flow to the heart. Another approach is to lower the heart’s demand for oxygen with drugs that reduce blood pressure or slow the heart rate.

Angioplasty or balloon angioplasty.
In this procedure, a catheter (a long thin tube) is inserted into an artery in an arm or leg and guided to the obstructed coronary artery. A second tube with a deflated balloon on its tip is passed inside the first, and the balloon is inflated where the artery is blocked. This enlarges its diameter by compressing the plaque. The procedure is relatively safe, but it does pose a 0.5-1 percent risk of death and a 3-5 percent risk of heart attack or stroke. The AHA has adopted new guidelines to improve these odds. They recommend that a patient have angioplasty at a hospital that performs at least 200 of these procedures every year and that are equipped to perform emergency bypass operations if the procedure fails. In addition, the physician doing the angioplasty should perform at least 75 of the procedures a year.
However, after a decade of enormous growth (between 1983 and 1992, the number of angioplasties performed each year rose from 26,000 to 400,000) the procedure’s effectiveness is being questioned. In about 25 to 50 percent of the people who’ve had angioplasty, the dilated part of the artery renarrows within the first six months. Some researchers also fear that forcing blood vessels open this way may cause damage that could actually increase the rate that new blockages develop. Yet, three or four angioplasties are often performed on the same area of an artery.
Before you have angioplasty, make sure you have had all the appropriate diagnostic tests, including an exercise stress test. Also ask about alternatives to it, such as life-style modification and medications.
Coronary Artery Bypass Graft Surgery (CABG). This procedure is usually recommended for patients with severe blockages of two or more of the major arteries to the heart. The surgeon takes a blood vessel from another part of the body (usually the leg or inside the chest wall) and constructs a detour around the blocked part of the coronary artery, thus restoring blood supply to the heart. As with any open heart surgery, there are significant risks associated with CABG. Moreover, a study by RAND, an independent research organization in California, suggests that about 10 percent of the 407,000 bypasses done each year are unnecessary.
There is good news: Researchers from California who analyzed findings from ten clinical trials, found that obstruction diminished, without requiring any invasive procedures, in nearly one third of people who followed strict programs to lower cholesterol with a low-fat diet, weight loss, regular exercise and drugs compared to one tenth of people who received less aggressive interventions.
Besides being the third major cause of death in the U.S., stroke is the principal cause of serious disability. A stroke occurs when a blood vessel to the brain bursts or is clogged by a clot or some other particle, depriving a part of the brain of oxygen. Nerve cells in the affected area cannot function without oxygen and die within minutes. The part of the body controlled by those cells can’t function either. The devastating effects of stroke, including paralysis and memory loss, are often permanent because dead brain cells aren’t replaced.
Warning Signs of Stroke
If you notice one or more of the following signs, see a doctor immediately.
- Sudden weakness or numbness of the face, arm or leg on one side of the body.
- Sudden dimness or loss of vision, particularly when it occurs in just one of the eyes.
- Loss of speech, or trouble talking or understanding speech.
- Sudden, severe headaches with no known cause.
- Unexplained dizziness, unsteadiness or sudden falls, especially along with any of the symptoms listed above.
| Myth: A heart attack feels like you’ve been stabbed in the chest and leaves you writhing on the floor in agony. Fact: Half of all people who have heart attacks wait two hours or longer before seeking treatment because they are not sure if their chest pain is caused by a heart attack. |
Also, about 10 percent of strokes are preceded by transient ischemic attacks (TIAs) or little strokes. TIAs occur when a blood clot temporarily clogs an artery, and part of the brain doesn’t get the blood it needs. The symptoms, very similar to those of stroke, occur rapidly and usually last less than five minutes. Unlike with a stroke, however, when a TIA is over the person returns to normal. Even though only about 36 percent of those who have TIAs later have a stroke, they are very strong predictors of stroke risk. So you should not ignore them. Prompt medical attention and clot-inhibiting drugs could prevent a fatal or disabling stroke from occurring.
Can a Stroke Be Prevented?
The best way to prevent a stroke from occurring is to reduce its risk factors, which include the same ones as heart disease in addition to the following:
- Heart Disease. Independent of blood pressure, people who have heart problems are at more than twice the risk of stroke than are people with normally functioning hearts.
- High Red Blood Cell Count. A marked or even moderate increase in the red blood cell count is a risk factor for stroke because such cells thicken the blood and make clots more likely. This problem can be treated by removing blood or administering blood thinning medications.
How Are Strokes Treated?
Treatments vary depending on the location, extent and cause of the stroke, but surgery, drugs, acute hospital care and physical rehabilitation may be necessary. For example, if a neck artery is blocked, surgery might be used to remove the buildup of plaque. This is called carotid endarterectomy. When a blood vessel has been blocked or blood clots are the problem, drugs may be used to help prevent new clots from forming. They can also keep an existing clot from getting bigger.
Sometimes treating a stroke means treating the heart. That’s because various forms of heart disease can contribute to the risk of stroke. For instance, damaged heart valves may require surgery or anti-clotting drugs to reduce the chance of clots forming around them. Such clots pose a possible danger since they could travel to the brain via the bloodstream and cause a stroke.
| Myth: I can feel it if I have high blood pressure. Fact: High blood pressure usually has no symptoms. In fact, many people have high blood pressure for many years without knowing it. |
Women and Heart Disease
Although many people think that men are the only ones who need to worry about cardiovascular disease, the fact is that about 30,000 more women than men die of it every year. While it is true that more men have heart attacks than women and men have them earlier in life, women have a poorer chance of survival. According to the AHA, 39 percent of women die within a year after having a heart attack compared to 31 percent of men. And during the first four years after a heart attack, 20 percent of women have a second one compared with 16 percent of men.
Clearly heart disease is an epidemic in women as well as in men. The main difference between the sexes is not whether women are likely to get heart disease, but when: Heart disease takes almost a decade longer to show up in women. Before menopause, women seem to be partly protected from the risk of heart attack, perhaps due to the hormone estrogen. After menopause, however, women’s risk of heart attack begins to rise steadily, reaching men’s in about ten years (See The Truth About Menopause for information about estrogen replacement therapy).
In addition, a woman’s symptoms are usually less severe and more confusing than those of a man. For example, in women, gallbladder disease and hiatal hernia symptoms can mimic those of heart disease. Also, women’s chest pain is more frequently the result of gas, muscle cramps, cartilage inflammation or anxiety. Women often report that symptoms of heart disease originated as pain in an adjacent area, such as an arm, shoulder, or the back, making it harder to diagnose.
| Myth: I am a woman so I don’t need to worry about heart disease. Fact: Heart disease claims the lives of about 30,000 more women than men every year. |
Until recently few studies have examined women’s risk for heart disease or how it is manifested in them. That’s why health care professionals know less about diagnosing and treating female heart patients than their male counterparts. Consequently, heart disease in women is likely to go undetected and untreated. If you suspect you have a heart problem, don’t hesitate to seek help. Go to the doctor and make sure you get the attention you need. If you have persistent symptoms of heart disease, don’t accept no for an answer. And if your doctor does not take your symptoms seriously, get a second opinion.
An Ounce of Prevention
The truth is that you can help prevent cardiovascular disease by improving certain lifestyle habits. A balanced diet low in fat, cholesterol and salt, in addition to regular aerobic exercise and regular medical screening will go a long way toward keeping your heart ticking properly.
Eating Smart
A lot of information, often contradictory, has been published about heart-healthy diets, so you may be confused as to what is good and what isn’t. Here is some straightforward advice to help you make smart food choices that could help you avoid heart problems later.
Cholesterol is a soft, fat-like substance that is found in all your body’s cells. It’s an important part of a healthy body because it’s used to form cell membranes, certain hormones and other tissues. However, too much cholesterol is dangerous to your heart and arteries.
Cholesterol comes from two sources: it’s produced by your liver, and it’s found in foods that come from animals, such as meat, poultry, seafood, dairy products and eggs. Egg yolks have high concentrations of cholesterol. Foods from plants don’t contain cholesterol.
Cholesterol travels to the body’s cells through the bloodstream but, like other fats, it cannot dissolve in blood. It has to be transported by special carriers called lipoproteins. There are several kinds of lipoproteins, but low density lipoprotein (LDL) and high density lipoprotein (HDL) are the cholesterol carriers so they are the ones to watch when it comes to heart disease.
LDL is the major cholesterol carrier in the blood. When a person has too much LDL-cholesterol circulating in the blood, it can slowly build up in artery walls. Together with other substances in the bloodstream it may form plaque, a thick, hard deposit that can clog arteries and lead to a heart attack or stroke. That’s why LDL-cholesterol is often called “bad” cholesterol.
About one-third to one-fourth of blood cholesterol is carried by HDL. Medical experts think HDL tends to carry cholesterol away from the arteries and back to the liver, where it is passed out of the body. That’s why it is often referred to as “good” cholesterol.
You should consume no more than 300 milligrams (mgs.) of cholesterol a day (one egg yolk has about 213 mgs. of cholesterol).
| Myth: Alcohol is good for the heart. Fact: While a glass of wine a day may raise good cholesterol slightly, heavy, regular consumption of alcohol can increase blood pressure dramatically. |
Fat is also an important factor because it can raise blood cholesterol levels. There are three kinds of fats in the foods we eat: saturated, polyunsaturated and monounsaturated fatty acids. Saturated fat is the main dietary culprit in raising blood cholesterol. Like cholesterol, it is found mostly in animal products, but it is also present in some plant products, such as coconut and palm oil, cocoa butter and heavily hydrogenated margarine.
The other two types of fat are unsaturated, and these are believed to help lower blood cholesterol, specially when used in place of saturated fat. They are found in vegetable oils, such as safflower, corn, and olive, as well as nuts, seeds and avocados.
The AHA recommends limiting your total fat intake to less than 30 percent of calories-with less than 10 percent from saturated fats.
Salt. Americans consume far more sodium (salt) than their bodies need. In some people who are sodium sensitive, too much salt can lead to high blood pressure. The problem: It is very hard to tell if you are sensitive to sodium. Because of this, it is best for everyone to moderate their salt intake by eating less than 3000 milligrams of sodium per day (one teaspoon of salt contains about 2,000 mgs).
Regular exercise does wonders for your heart. Don’t forget, your heart is a muscle and, like any muscle, it needs to be exercised to stay in top shape. Aerobic exercise-rhythmic movement sustained for at least 20 minutes-improves the ability of your heart, lungs and blood vessels to use oxygen. Such workouts also increase the heart’s pumping capacity so that it has to work less hard during every day activities. Think of it as an engine that can go up to 200 miles an hour, for which riding down the highway at 60 is practically effortless.
In addition, aerobic exercise, such as jogging, aerobic dancing, brisk walking, and bicycling, increases your body’s ability to burn calories, particularly from fat. Thus, you can avoid another heart disease risk factor: obesity. Regular aerobic activity also seems to increase the “good” cholesterol (HDL) and lower blood pressure.
To condition your heart and lungs, The AHA recommends 30-60 minutes of exercise 3-4 times a week. During each session, work hard enough to bring your heart rate to within the target heart rate zone, but not so hard that you are out of breath (during the ideal aerobic state you break a sweat but you can still converse freely). Your target heart rate depends on your age and maximum heart rate. Usually your maximum heart rate is determined by subtracting your age from 220. Your target heart rate zone is 60-75 percent of your maximum heart rate (see chart).
| Myth: You need to exercise long and hard for it to do any good. Fact: Even modest levels of low-intensity physical activity, such as walking, gardening, housework and dancing, are beneficial if done regularly and long term. |
Check if you are within your target heart rate zone by taking your pulse immediately after you stop exercising. To do so, place the tips of your first two fingers lightly over the artery on your neck and count your pulse for 10 seconds. Then multiply that number by six. If the result falls within your target zone, you’re doing fine. If it’s below, exercise a little harder next time, and if it’s above it, exercise a little easier. Never try to exercise at your maximum heart rate.
Heart-Saving Tests
You should have regular check-ups to monitor any changes in your heart, blood pressure or cholesterol levels. The following are diagnostics tests commonly used for this purpose. Some are used regularly, while others should only be done if symptoms of heart disease, such as shortness of breath or chest pain, are present or other tests point to a problem.
1) Blood Pressure Test. High blood pressure can damage your heart, lungs, brain and kidneys before you are even aware of it because high blood pressure usually doesn’t have symptoms. It doesn’t make you feel tired, weak, grumpy or tense, making this simple, fast and painless test vital. A doctor or nurse uses a stethoscope and a pressurized cuff wrapped around your arm to measure the pressure in an arm artery at two different times: during a heartbeat (systolic pressure) and between beats (diastolic pressure). For most adults, a blood pressure reading that’s less than 140/90 means there’s no cause for alarm.
2) Cholesterol Test. There are two types of cholesterol to check. The first provides a single measure of all types of cholesterol in your blood. A total cholesterol test is quick and easy and requires only a drop of blood. If your total cholesterol level is less than 200 mgs/dl, that is considered to be good. 200 to 239 is borderline high and over 240 is too high. The AHA recommends that everyone over 20 have their blood cholesterol checked every five years.
If your total blood cholesterol exceeds 200, a cholesterol fractions test may be warranted. This test, which requires you to fast before having a blood sample drawn, provides measures of HDL- and LDL-cholesterol, guiding your doctor’s recommendations.
3) Diabetes Test. Over time, diabetes can cause heart trouble and stroke, among other problems. If diabetes runs in your family or you develop classic diabetes symptoms, including fatigue, excessive thirst, frequent urination and blurred vision, you should ask your doctor to perform this simple urine test.
4) Electrocardiogram (EKG). An EKG can reveal irregular heart rhythms. This is done by attaching sensors, which transmit the heart’s electric impulse to a recording device, to various points on the patient’s chest. Having a baseline EKG can be helpful in determining whether any chest pain is due to a heart attack or another less severe condition.
5) Exercise Stress Test. Also known as an exercise EKG, this test records heart rhythms while a person walks on a treadmill or pedals a stationary bicycle for a given length of time at a specific speed. It is important in the diagnosis of heart disease because sometimes abnormal changes in cardiac function, such as angina, are absent during rest but they may appear with exercise.
6) Chest X-ray. Gives a cursory look at the person’s lungs and the size and shape of the heart.
7) Echocardiogram. A painless test that uses high-frequency sound waves to image the heart’s internal structures. A Doppler Echocardiogram uses sound waves to measure blood flow. By combining these two tests, doctors can learn about the heart’s structure and function.
8) CT Scan. A Computed Tomography is an x-ray technique that produces a film representing a cross section of tissue structure.
9) Coronary Angiography. If you have symptoms of heart disease, your doctor may order this invasive, but generally painless procedure. The cardiologist threads a long, thin tube called a catheter through a major artery in your arm or leg and then into a coronary artery. A special dye that an x-ray can “see” is then injected into the coronary artery and a series of images are made. Doctors can then determine if the blockage poses an immediate threat.
Also known as a cardiac catheterization, this test is often used to evaluate other problems, such as poorly functioning heart muscles, diseased or damaged heart valves and congenital heart defects. But this test does pose a 1 in 100,000 risk of death and a 1 in 10,000 risk of stroke or heart attack. If complications do develop, you might need immediate open-heart surgery. Therefore, the American College of Cardiology recommends angiocardiography be performed in a hospital that performs a minimum of 300 Angiocardiographies a year.
Our thanks to C. Noel Bairey Merz, M.D., Director, Preventive and Rehabilitative Cardiac Center, Cedars-Sinai Medical Center, Los Angeles, CA, for reviewing this article.
Heart Attack: No Time to Spare!
When it comes to a myocardial infarction, or heart attack, time is of the essence. Most of the permanent damage done to the heart occurs during the first hour. Yet half of all people who have heart attacks wait two hours or longer before seeking treatment because many of them don’t realize what’s wrong. They incorrectly assume the symptoms of a heart attack are so severe they will immediately fall to the floor in agony if they have one. In fact, heart attacks often feel like bouts of indigestion or heart burn. Knowing how to recognize a heart attack when it occurs could save your life.
Heart Attack Warning
Despite popular belief, a heart attack is not a one-time event. It is a process that develops over hours as the heart’s tissue is destroyed by lack of oxygen. Such damage causes the following symptoms (the AHA cautions that you may not feel them all and those you do feel may come and go):
- Uncomfortable pressure, fullness, squeezing or pain in the center of the chest that lasts more than a few minutes, or goes away and comes back.
- Pain that spreads to-or occasionally originates in-the shoulders, neck, lower jaw or arms.
- Chest discomfort with light-headedness, fainting, sweating, nausea or shortness of breath. Sharp, stabbing, short twinges of pain are usually not signals of a heart attack. In addition, about half of all heart attack victims have warning symptoms hours or weeks in advance. The earliest predictor of an attack is recurrent chest pain triggered by physical exertion and alleviated by rest.
Every Second Counts
The best way to prevent progressive damage is to start treatment with clot-dissolving medications as soon as possible. These drugs destroy the clot and restore blood flow to the heart. A University of Washington study found that 75 percent of people survived heart attacks with little or no heart damage when treatment with these drugs was started within 70 minutes of the onset of symptoms. An emergency angioplasty can also be performed to widen blocked arteries and allow blood to flow more easily. But its effectiveness diminishes after two hours as well.
Don’t waste these precious minutes trying to decide if your discomfort indicates a heart attack or not. If you have any of the above symptoms for more than a few minutes:
1) Call 911 immediately. If you want to call your physician, do so after calling your local emergency response system first (if the 911 system is not available in your area and you do not know the local emergency number, ask the operator to connect you). Describe your symptoms when you call. This will ensure a priority dispatch of paramedics trained in cardiac life support.
2) Decide on the fastest method of transport. Ask the dispatcher how long it will take emergency workers to get you to a hospital. If you can get there faster by going yourself, have someone drive you. Don’t try to drive yourself.
3) Chew aspirin. Aspirin inhibits blood clotting and, according to the Mayo Clinic, when taken during a heart attack it can decrease death rates by about 25 percent. Chewing a regular-strength aspirin will speed absorption.
Eating Plan Tips
To help you adhere to a heart-healthy diet, the American Heart Association offers the following tips:
- Eat no more than 6 ounces (cooked) per day of lean meat, fish and skinless poultry.
- Eat 5 or more servings of fruits and vegetables per day.
- Eat 6 or more servings of breads, cereals or grains per day.
- Try main dishes featuring pasta, rice, beans and/or vegetables. Or create “low-meat” dishes by mixing these foods with small amounts of lean meat, poultry or fish.
- Use no more than 5 to 8 teaspoon servings of fats and oils per day for cooking and baking, and in salad dressings and spreads.
- Use cooking methods that require little or no fat: boil, broil, bake, roast, poach, steam, sauté, stir-fry or microwave.
- Trim off the fat you can see before cooking meat and poultry. Drain off all fat after browning. Chill soups and stews after cooking so you can remove the hardened fat from the top.
- Limit your consumption of egg yolks to 3 to 4 per week. This includes those used in cooked and baked products, whether home-made or store-bought.
- Restrict your use of organ meats such as liver, brains, chitterlings, kidney, gizzard, and sweetbreads. They are very high in cholesterol.
- Choose skim or 1% fat milk and nonfat or low-fat yogurt and cheeses.
- For low fat recipes call the National Cholesterol Education Program at 800-575-WELL.
Heart Rate Target Zone
To benefit most from aerobic exercise, it is important to maintain your heart rate within the recommended target zone while you exercise. Your target zone is 60 to 75 percent of the maximum heart rate recommended for someone your age. Both are listed above. To see if you are within your target zone, take your pulse at intervals during exercise. Count your heart beats for 10 seconds and multiply by six.
| Age (years) | Heart Rate Target Zone beats/minute) | Average Maximum Heart Rate (beats/minute) |
| 20 | 120 – 150 | 200 |
| 30 | 114 – 142 | 190 |
| 40 | 108 – 135 | 180 |
| 50 | 102 – 127 | 170 |
| 60 | 96 – 120 | 160 |
| 70 | 90 – 113 | 150 |




